Also known as frontotemporal dementia (FTD), it refers to a form of dementia that is characterized by the progressive degeneration of the brain’s frontal and temporal lobes. It mainly affects brain areas responsible for executive functions, behavior, language, and personality. According to the National Institute on Aging, FTD tends to occur at a younger age than other forms of dementia, and it’s usually rare. 60% of people from ages 45 to 64 years old have FTD. This condition is progressive, in which symptoms can get worse over time.
People just have one symptom in the early stages. But other symptoms can appear as the disease progresses due to the numerous parts of the brain that can be affected. Determining how long an individual can live with a FTD condition is difficult. Others live less than two years after diagnosis, while some live for more than 10 years after diagnosis. If you have frontal lobe dementia, receiving a proper diagnosis from a medical professional specializing in neurodegenerative disorders is essential. In this blog post, we’ll discuss the potential causes, symptoms, and treatment for FTD so you can spread awareness and educate others.
What are the causes of frontal lobe dementia?
Cause No. 1: Environmental factors
These factors have been suggested as potential contributors to the development of frontal lobe dementia or frontotemporal dementia (FTD). But their particular interactions and roles aren’t yet fully understood. Particularly severe or repetitive injuries or a history of significant head trauma have been associated with an intensified risk of having FTD. Accumulation of abnormal proteins in the brain can result from traumatic brain injuries, including TD-43 and tau, which are FTD pathology characteristics.
Significant or prolonged exposure to particular environmental chemicals or toxins can potentially increase the possibility of having FTD. Occupational exposures associated with a higher risk of developing FTD include exposure to pesticides, metals, and other chemicals. Moreover, some research suggests that bacterial or viral infections can play a role in the development of FTD. For example, herpes simplex virus type 1 (HSV-1) has been associated with some FTD cases. The infection can lead to neuronal damage and the onset of FTD symptoms since it can trigger an inflammatory response, according to a hypothesis.

Cause No. 2: Genetic Mutations

According to the University of California San Francisco’s Weill Institute for Neurosciences, genetic FTD is passed down in families in a dominant pattern. When a child of a person who has an FTD-causing gene mutation has a 50 percent or 1 in 2, the occurrence of the same mutation is possible. Nearly every person with an FTD-causing gene mutation will develop a related condition (if not FTD) if he lives until the 8th decade as an exception. Depending on which FTD-causing gene mutation is present, the usual age of the first symptom varies.
Mutations in the microtubule-associated protein tau (MAPT) gene are strongly associated with tauopathy, a subtype of FTD. These mutations lead to tau protein aggregation and abnormal processing, which forms neurofibrillary tangles in the brain. These tangles contribute to the degeneration of neurons in the frontal and temporal lobes and disrupt normal cellular function. Even progranulin (GRN) mutations are associated with an FTD subtype characterized by a progranulin protein deficiency.

Cause No. 3: Protein abnormalities
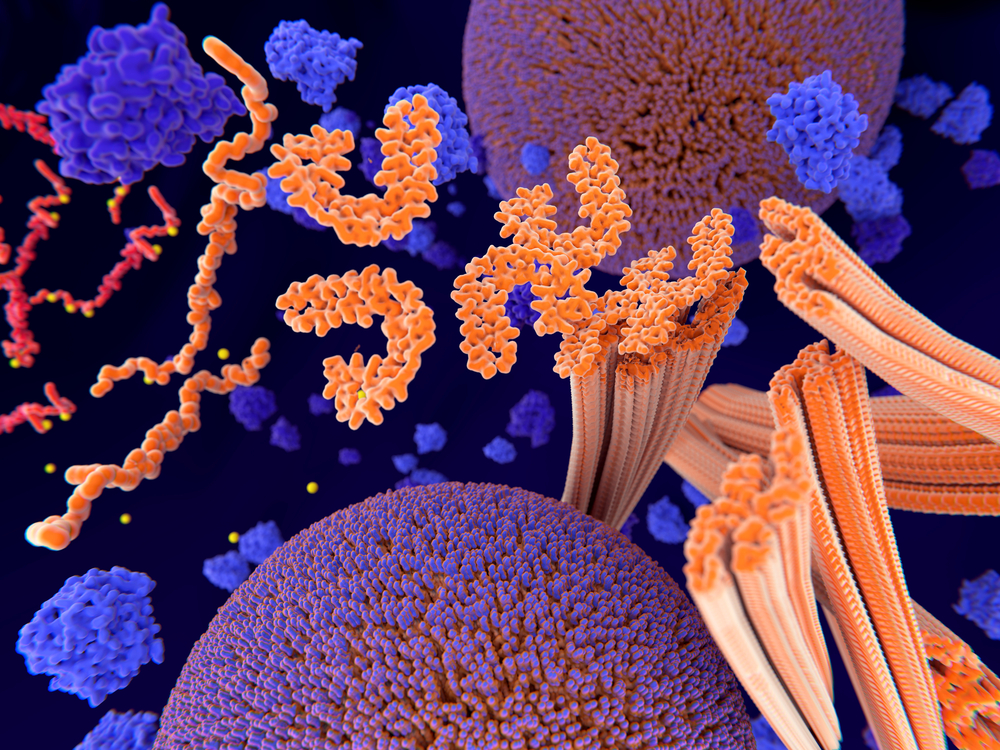
According to Stanford Health Care, there is an abnormal tau protein form in the brain that can be found in approximately 50% of people with FTD. At the same time, 50% of people have TDP-43 protein accumulation if they have FTD. There are also 5% of people who have FUS protein accumulation. This may cause cells to die and can disrupt normal cell activities. Tau protein is involved in stabilizing microtubules, which are important structures for maintaining the function and structure of nerve cells. Abnormal tau proteins in the brain can lead to the formation of neurofibrillary tangles in specific FTD subtypes.
TDP-43 protein forms and accumulates aggregates in brain regions that are affected, based on a significant portion of FTD cases. These TDP-43 aggregates contribute to neurodegeneration, disrupting cellular processes and impairing the functions of nerve cells. Also, fused in sarcoma (FUS) is another implicated protein in FTD. The FUS gene and its mutations can cause FTD symptoms by leading to abnormal accumulation of FUS protein in the brain.

What are the symptoms of frontal lobe dementia?
Symptom No. 1: Decline in empathy and social awareness

A 2013 study published in the National Library of Medicine shows that behavioral variant frontotemporal dementia (FTD) is associated with apathy, loss of social tract and propriety, social disengagement, disinhibition, and loss of sympathy or empathy with others. The diagnosis for this condition depends on clinical criteria, which include alterations in emotional and social behavior with the supplement of frontotemporal changes in neuroimaging.
On the other hand, social cognition refers to the ability to understand social norms, interpret social cues, and navigate social situations appropriately. You may have difficulty recognizing and interpreting social cues like body language and facial expressions with an FTD condition. You may struggle to comprehend subtle social cues or misinterpret the intentions and emotions of others.

Symptom No. 2: Executive dysfunction

It’s important to note that executive functions are cognitive processes that help individuals make decisions, problem-solve, plan, organize, and initiate and inhibit behavior. According to Northwestern Medicine, failure of executive functions can increase safety risks since they may be unable to inhibit inappropriate actions or plan appropriate actions. Individuals with frontal lobe dementia usually lack flexibility in thinking and can’t carry a project consistently toward completion.
If you have FTD, you may have difficulty creating and following schedules, setting and achieving goals, and managing time efficiently. This can lead to an inefficient and disorganized approach to tasks, resulting in difficulties in carrying out daily routines. Moreover, you may have a reduced ability to initiate and carry out tasks or activities independently. To start and complete the tasks, you may require increased reminders, prompting, and assistance.

Symptom No. 3: Behavioral changes

These are prominent symptoms of frontal lobe dementia, specifically in the behavioral variant frontotemporal dementia (bvFTD). These changes can play a crucial role in regulating behavior and personality when they arise due to the degeneration of frontal lobes. If you have FTD, you may exhibit disinhibited behavior and reduced impulse control. You may engage in impulsive actions without considering the consequences, like making socially unacceptable or inappropriate comments, showing a lack of restraint in social situations, and engaging in risky behaviors.
Moreover, this condition can lead to a decline in interest, initiative, and motivation in previously enjoyed activities. You can become indifferent to your surroundings, have difficulty initiating and sustaining tasks, and show reduced engagement in work or hobbies. You may even notice changes in social behavior or interpersonal relationships. Some individuals can develop compulsive or repetitive behaviors. These behaviors can manifest as rituals, obsessions, or repetitive movements.

Symptom No. 4: Language difficulties

According to UCSF Health, the first symptoms of FTD are usually antisocial or unusual behavior and loss of speech or language. In the form of a primary progressive aphasia (PPA) as an FTD subtype, language difficulties can be a significant symptom of frontal lobe dementia. You may experience difficulty finding and retrieving words. It’s possible that you can struggle to use vague or circumlocutory language, recall common words, or substitute words with unrelated or incorrect ones.
Moreover, FTD can affect the ability to use correct grammar and syntax. You can face difficulty constructing sentences, maintaining appropriate sentence structure, and producing grammatically correct sentences. You can exhibit errors in pronoun usage, verb tenses, and word order. This symptom is also related to difficulty comprehending complex sentences, grasping the meaning of a written text, and following conversations.

What are the treatments for frontal lobe dementia?
Treatment No. 1: Speech and language therapy

According to Psychiatria Danubina, speech therapies offer a variety of treatments and methods for people with FTD. These include speech and language exercises and activities related to reading, repetition, and naming. They implement these activities through cognitive rehabilitation interventions and compensatory strategies. Speech therapists work closely with other medical professionals to determine the specific language deficits associated with FTD.
Moreover, speech therapies provide individuals with strategies to improve communication. This can include using cue cards, communication boards, and visual aids to facilitate conversation and support word retrieval. They may also want to work on strategies for language difficulties compensation, such as using gestures or context to aid understanding, paraphrasing, and circumlocution.

Treatment No. 2: Supportive care

This focuses on providing a supportive environment and addressing the unique challenges and needs faced by individuals with FTD and their caregivers. Providing education and information about FTD is necessary for both individuals with FTD and their caregivers. This can include understanding the nature of the disease, its progression, and the commonly associated symptoms. Education can help individuals, and their families anticipate challenges, develop coping strategies, and make informed decisions.
Psychosocial and emotional support is also crucial for individuals with FTD and their caregivers. Therapy sessions, support groups, and counseling can help individuals and families address grief and loss, develop coping mechanisms, and navigate the emotional impact of the disease. Modifying the environment to suit the needs of individuals with FTD can help optimize their functioning and minimize distress. This can include reducing environmental stimuli and distractions, creating a structured and predictable routine, and ensuring safety measures.

Treatment No. 3: Medications

Medications are often used in treating FTD to manage particular symptoms and improve the individual’s quality of life. But it’s important to note that no medications are specifically approved to treat FTD or slow the condition’s progression. But selective serotonin reuptake inhibitors (SSRIs) like citalopram and sertraline are usually prescribed to manage mood disturbances and depressive symptoms of individuals with FTD. These medications can help alleviate feelings of irritability, anxiety, and sadness.
Moreover, risperidone and quetiapine are atypical antipsychotic medications that may be prescribed to manage severe behavioral symptoms, psychosis, or agitation in FTD. But remember that using antipsychotics in FTD requires careful consideration because of its potential side effects, specifically in terms of increased mortality risk and movement disorders.

